Vaccine Update
We can see how the US (and Georgia) is doing with respect to the vaccine administration effort using the CDC’s COVID-19 Data Tracker understanding that delayed reporting can affect the numbers. Nationally, 62% of the available doses have been administered, either as a first or second dose. And Georgia’s usage rate is the same, 62.5%. While we wait for supply to increase, it is vital that we make the most use of the vaccine we *do* have. So, of course, I would prefer to see that percent administered be much, much higher. Hopefully the remaining doses have an appointment to meet their recipient in the coming days. Of those who have started the vaccine series, 22.4% have had their second dose. In long term care facilities (LTCFs), there have been 3.68 million doses administered (of the 31.1 million administered overall so far). Vaccine administration in LTCFs is one area where Georgia is doing rather well. The CDC COVID-19 Vaccine Tracker does not give us LTCF administration adjusted for population, but in terms of people in LTCFs with two doses of the vaccine, Georgia is ranked the #15 state in the nation, at 9424 people.
Georgia’s vaccination rate has increased 43.6% in the past week, which is good news but not as good as the previous week. For the state, 766,875 people have initiated the two-dose series, which is more than the cumulative number of COVID-19 cases that Georgia has recorded (a cool milestone!). And we did that in about 6 weeks! 119,878 people have completed the 2-dose series in Georgia (1.1% of the GA population). It is great to see that upward momentum. Georgia is still ranked in the bottom half of the US, but moved up from #32 to #28 in the nation this week, with a 1+ dose vaccination rate that is 7223 per 100,000 residents. Perhaps next week we will be in the top half of the states. The top three states for first doses administered per 100,000 residents are Alaska (12971), West Virginia (10746), and Connecticut (9813). The bottom three states are Idaho (5500), Missouri (5551), and Iowa (6044). This week, Georgia has administered 1+ doses per 100,000 at a rate that is 44% less than the leader (Alaska). But last week the difference was 53% higher. So we’re continuing to narrow that gap and improve.
The World
According to the New York Times Coronavirus Tracker, the SARS-CoV-2 virus that causes COVID-19 disease has sickened >102.9 million people (+3.5 million since last week) and killed at least 2,226,700 (+92,700 in the past week) worldwide as of this morning. Those are big weekly numbers. But believe it or not, they are better than we’ve seen in recent weeks.
Things have improved this week for many countries in terms of average daily cases per 100,000, including the UK and South Africa where two of the more transmissible variants come from. We are ranked #13 in the world for average daily case rate per 100,000 people over the past 7 days (same as last week) with a rate of 45 compared to 51 last week. So our case rate has improved. The top five countries for average daily case rate per 100,000 in the past week are Portugal, Turks and Caicos Islands, Montenegro, Spain and Israel.
For deaths, the US average daily death rate per 100,000 over the past week is 0.95 (previous week was 0.93), and we are ranked #12 in the world for this (last week we were ranked #17). The top five countries for average daily death rate per 100,000 in the most recent week are Gibraltar, Portugal, United Kingdom, Lebanon and Slovakia.
The United States
The map above comes from the New York Times Coronavirus Tracker. As of this morning, there have been over 26.2 million cases (+2.3 million in the past week) and 441,296 deaths in the US (+43,684 in past week). Keep in mind that both of these numbers are probably an under-count of the situation in our country.
This week things are a lot better for many areas. It’s most noticeable in the four corners region (Utah, Colorado, New Mexico and Arizona). But we also see a lot of improvement through the Midwest to northeast as well as in the northern half of Georgia. According to data from the 31Jan21 HHS Community Profile Report (the source document for the White House Coronavirus Task Force reports), the top five states in the nation for new case rate per 100,000 residents are Arizona, South Carolina, Rhode Island, New York and Texas. Georgia is close behind at #6. South Carolina and Georgia are joined by North Carolina (#9) as the Southern states in the top 10. The top five states in the nation for average daily death rate in the past 7 days are Alabama, Arizona, Tennessee, South Carolina and California. In addition to Alabama (#1), Tennessee (#3) and South Carolina (#4), other Southern states in the top 10 include Mississippi (#6) and Georgia (#8).
The table below tells you where we are this week and how that compares to the previous week (in parentheses). The data for everything comes from the HHS Community Profile Report from 31Jan2021.
Georgia is steady for death rate per 100,000, but its ranking has decreased by 3, meaning that things are worse elsewhere. Georgia currently has one county (Chattahoochee) in the list of the top 20 counties for disease rate in the nation and it is ranked #1.
Influenza-like illness in almost all of the US remains minimal, but Tennessee is in the “low” category (next level above minimal). You can consult FluView any time you’d like to see this map and other data visualizations. You can read the weekly report from Georgia Department of Public Health here.
Since flu isn’t such a big deal this year (yay! Good job!), I’d like to take another look at excess deaths, something we haven’t looked at for a while. The graph below looks at US weekly death totals for all causes (blue bars). The green bars are weekly deaths if the COVID-19 deaths are subtracted out. Of course, all the bars are green prior to the pandemic since COVID-19 wasn’t a thing then. The orange line is the threshold for what is considered to be the normal seasonal trend. When deaths spike above the orange line, they are considered “excess” deaths, relative to what we were expecting.
We can see that the COVID-19 pandemic isn’t the only time in recent history that we’ve spiked above that excess threshold - we did so in January 2018 too. That was a particularly bad year for seasonal influenza. As we can see in the past year, the impact of COVID-19 has dwarfed the impact of seasonal influenza, both in terms of intensity as well as duration. As far as death surges go, the summer surge was the lightest one of the three that the US has experienced so far, even if it was particularly bad for the South. But the winter surge looks like it will be the deadliest of the three so far, since it is already at the same level as the spring surge and we know that deaths continue to remain high and death reporting can be delayed by as much as 8 weeks.
For COVID-19 burden on hospitals, things have improved a lot for the northern half of the US, but remain intense in the southern half of the country and along the eastern seaboard. Georgia and South Carolina are especially hard hit among Southern states. The next two maps/graphs come from the 31Jan2021 Community Profile Report (PDF summary document).
And that agrees with what we see for new hospital admissions per 100,000 residents. The rate is decreasing nationwide, but the winter peak was most intense for Southern states and it remains higher than the rest of the country even while it is decreasing. Notably, we also had the most intense admission rate during the summer surge.
Georgia
The biggest piece of news to come out of Georgia today is that Georgia DPH told us that they have now identified 19 cases of the UK variant in Georgia. They have been found in Georgians ranging in age from 15 - 61, in 8 males and 11 females. They have been found in 9 Georgia counties including Atlanta (Fulton and DeKalb), Atlanta Suburbs (Cherokee, Clayton, Cobb, Douglas, Gwinnett), and two nonrural counties outside of the Atlanta metro (Carroll and Paulding). You can see from the map below that these are all clustered together near the Atlanta metro.
I’ve already sat for a couple media interviews for this topic, so let me offer the same insights here. If you are in one of these counties, I do not think you need to panic. However, if you have become lax in following the public health recommendations for limiting disease transmission, let this be an important reminder to you to get back on board with this team effort. The same things we have been recommending this whole time will work here too:
Avoid indoor gatherings
Avoid large gatherings
Avoid any indoor activity with non-household contacts where masks cannot be worn (this is unsafe for any age group). This includes eating and drinking. Love your local restaurants with meal delivery or carry out (and tip big), but indoor dining is one of the most dangerous things you can do right now.
Ensure you are wearing a well-fitting mask when around non-household contacts, especially when indoors. Ideally, cloth masks should be made of 3 layers. You can also consider layering masks together, such as a surgical/procedure mask under a cloth mask, or wearing a KN-95 mask. But the most important thing here is that your mask fits and there is little to no gap along the edges between the material and your face.
Cover your coughs and sneezes with your elbow. Wash your hands frequently. Use hand sanitizer if soap and water are not available.
Stay home if you’re feeling ill and be on the lookout for COVID-19 symptoms. Flu activity is minimal this year and the common cold is no longer common either. Seek a COVID-19 test if you are having cold or flu-like symptoms.
Chances are good that this variant has been circulating in Georgia for weeks. Georgia and the US more broadly are only screening a very tiny percentage of all COVID-19 positive specimens for the variants. At least two cases of the South African variant have been detected next door in South Carolina. In today’s press release, Dr. Toomey said she thought the UK variant would be the dominant strain of the virus in Georgia by March.
These variants are more transmissible. They have a mutation on their spike protein that makes them stick more tightly to the receptors on our cells. So far, the vaccine manufacturers have indicated that their vaccines are successful against these variants. So that is reassuring.
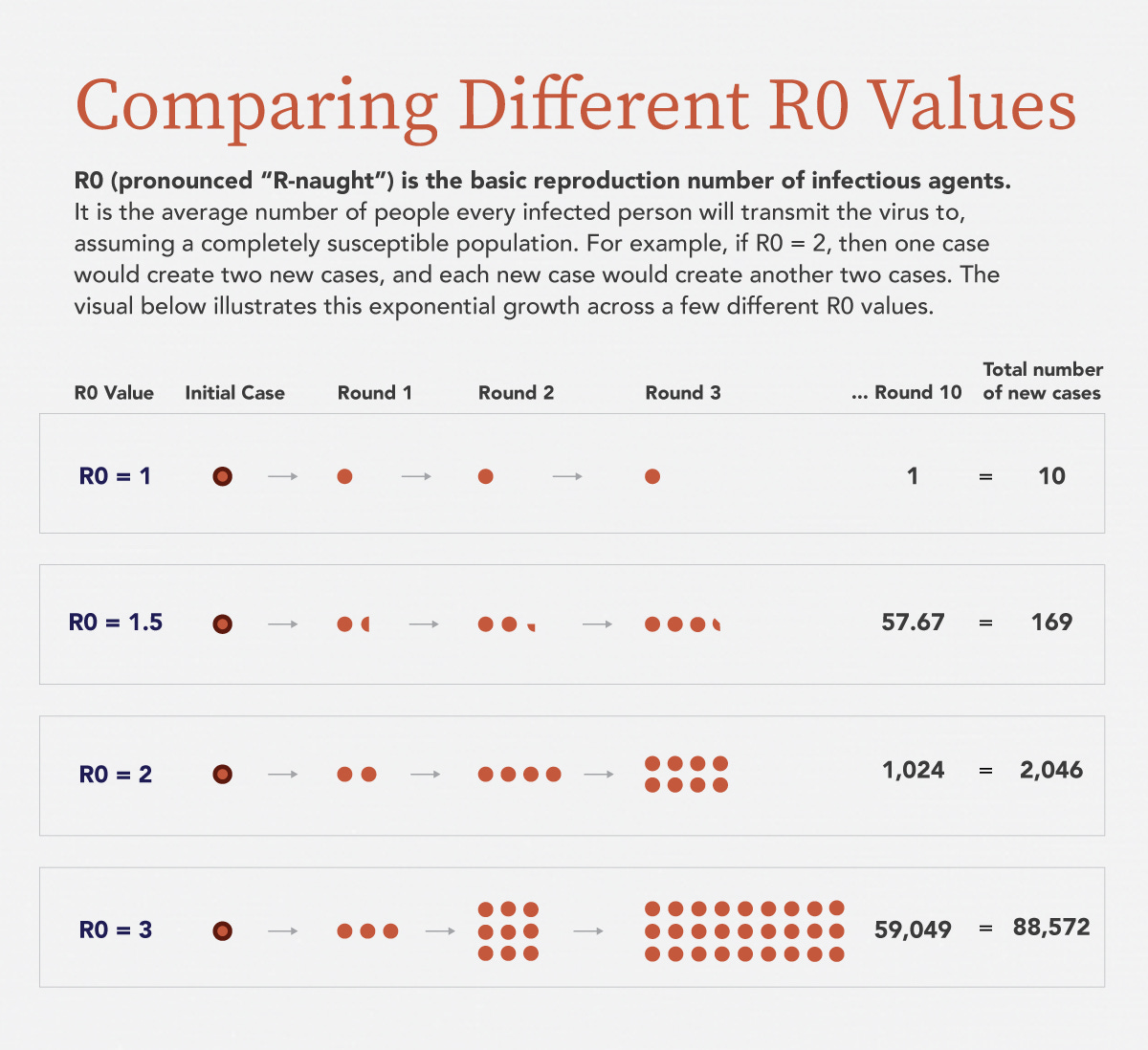
But let’s dig deeper into what I mean when I say something is more transmissible. The R0 value is an estimate that in a community that has never seen a disease before (i.e. COVID-19), how many people can one person infect. Things get muddier now since we don’t have a completely susceptible population (a lot of people have been infected or have been vaccinated). But it helps us to have a thought experiment for now. You can read my thoughts on a related estimate called Rt here. The R0 for COVID-19 has been estimated to be about 2.5 according to CDC. So a person sick with COVID-19 on average goes on to infect 2.5 people. Using the table below, let’s just round down to 2 for now. Eventually, a chain might start to grow of infected individuals from that initially infected person, and the virus goes through 10 rounds of this in our thought experiment. At the end of the 10th round there are 2046 sick individuals. Using Georgia’s rates, 112 of those folks need a hospital, 34 people will die.
The R0 for the UK variant is estimated to be 40-80% higher than the wild type version of SARS-CoV-2 we’ve been experiencing thus far. Let’s take the low end estimate (40%) and now the R0 is 3.5. We’ll round down as we did before so that the graphic above works for this illustration. Just understand that this might be the best case scenario. If we run through the same simulation as we did before, with 10 successive rounds of infection among connected individuals, at the end of 10 rounds we have 88,572 sick individuals. Using Georgia’s rates for hospitalization and death, that would predict 4871 hospitalizations and 1488 deaths. That’s a much heavier burden for hospitals and a much higher toll for families who lose loved ones. It’s not that the virus itself is more deadly to the person who is infected. It’s more of a shots-on-goal artifact. The hospitalization rate and mortality rate is the same, but there are more people infected with the virus, so more hospitalizations and more deaths.
I know these are scary numbers though. For those who have had the ability to work from home or shelter in place, your life probably isn’t going to change that dramatically. But we need for you to keep doing what you’re doing. This variant is going to be more risky for essential workers in high public contact jobs. It makes the need to vaccinate people as quickly as possible even more important. But because we don’t have enough vaccines yet to vaccinate everyone who wants one, we need EVERYONE to do better at recognizing the threat COVID-19 poses to our communities and be part of the effort to limit disease transmission. Stay out of the transmission chain as much as you can both for your sake and for essential workers. When you make a decision to get takeout instead of eating in a restaurant, you interrupt that lineage of infections in the graphic above. When you gather outdoors and socially distanced from friends, rather than indoors to watch the SuperBowl, you interrupt transmission. The people we save from infection, hospitalization and death through seemingly minor adjustments adds up quickly.
Let’s discuss today’s numbers for Georgia.
Testing: a lower day for PCR testing, not unusual considering it is a Monday. There were 21,387 new PCR results reported, 14.4% of which were positive. Antigen testing identified 14.9% of today’s cases.
Cases: cases are often lower on Mondays due to weekend effect. Today there was a net increase of 3034 newly reported cases (2581 by PCR, 453 by antigen test). Of today’s newly reported cases, 33.2% came from nonrural counties outside of the Atlanta metro followed by Atlanta suburb counties with 30.9%.
Hospitalizations: there are 4094 patients currently hospitalized for COVID-19. This is a decrease of 16% compared to a week ago. According to the HHS Community Profile Report, the top 5 counties for percentage of inpatient beds occupied by a COVID-19 patient are Dodge, Crisp, Bacon, Pickens and Liberty counties.
COVID-19 patients represent 29.6% (-13% since last week) of all patients currently hospitalized in Georgia and this varies by hospital region. None of the 14 hospital regions in Georgia have a COVID-19 patient percentage compared to all inpatients above 40%. Last week there were 2. In fact, we now have two regions (J and newcomer L) who have moved down from dark red zone to light red zone (small victories are still victories!). Georgia is #3 in the nation for this metric behind Arizona and California.
85.1% of the ICU beds in the state are full. According to HHS, 43% of Georgia’s ICU beds are occupied by COVID-19 patients and we are tied for #2 in the nation for this metric with Texas and Alabama. None of Georgia’s hospital regions are coping with an overage demand of ICU beds. Five regions (of 14) are using >90% of their ICU beds. Last week, it was 8 regions. So there are several signs of improvement here.
There were 86 new hospital admissions for COVID-19 today and 1 admission to the ICU. We typically see lower numbers on Mondays.
Deaths: there were 43 newly reported confirmed deaths compared to yesterday’s total. Death reporting on Mondays is typically low due to weekend effect. For today’s deaths, 48.8% came from nonrural counties outside of the Atlanta metro and 27.9% came from rural counties. Eighteen percent of today’s deaths came from the Atlanta suburbs and 2% came from the Atlanta counties of Fulton and DeKalb. The state 7-day death rate per 100,000 residents is 30.6% higher than the summer peak.
References
https://covid.cdc.gov/covid-data-tracker/#vaccinations
https://beta.healthdata.gov/download/gqxm-d9w9/application%2Fpdf
https://dph.georgia.gov/covid-19-daily-status-report
https://covid-gagio.hub.arcgis.com/
https://www.cdc.gov/nchs/nvss/vsrr/covid19/excess_deaths.htm
https://dph.georgia.gov/press-releases/2021-02-01/increased-cases-covid-variant-b117
https://www.mastersindatascience.org/resources/r0-infectious-diseases/
https://www.cdc.gov/coronavirus/2019-ncov/hcp/planning-scenarios.html
Georgia COVID-19 Updates is a free newsletter that depends on reader support. If you wish to subscribe please click the link below. There are free and paid options available.
My Ph.D. is in Medical Microbiology and Immunology. I've worked at places like Creighton University, the Centers for Disease Control & Prevention and Mercer University School of Medicine. All thoughts are my professional opinion and should not be considered medical advice.