Week in Review, 17-23May2021
Georgia COVID-19 Updates
Combined Data
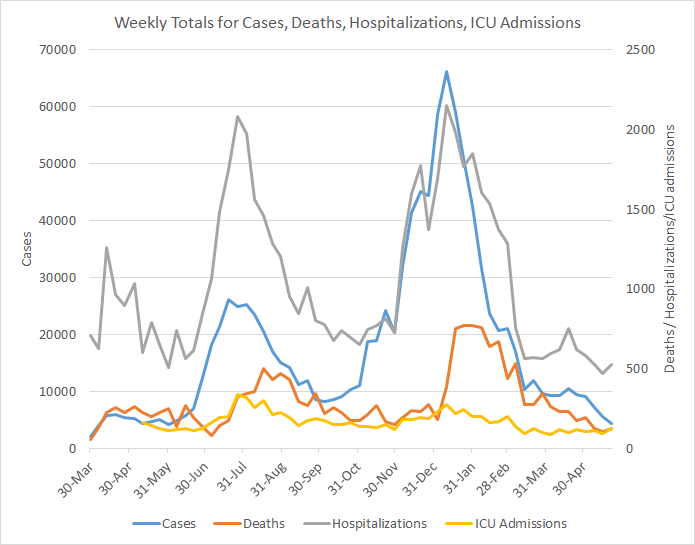
The graph below shows how four of our big metrics for tracking the COVID-19 pandemic are tracking over time. Cases are represented by the blue line and correspond with the left y-axis. All other metrics correspond with the right y-axis. The reason I graph all of these things together is so that we can see the way these things trend together (or differently) over time.
After several weeks of decline, we are seeing an increase in three of the four metrics: deaths increased 22%, hospitalizations rose 12% and ICU admissions rose 31%. Cases declined by 22%. Some of these metrics, especially deaths and ICU admissions often have a lot of variation. Hospitalizations have had bumpy roads down to a baseline too. Take, for example, what happened after the summer surge last year. These increases could just be that same situation where we might expect to see the numbers resume their declines next week. It’s just something for us to keep an eye on. Last year, we think Georgia’s summer surge began as the result of pandemic fatigue and Memorial Day gatherings. Let’s hope that we have vaccinated enough people to prevent another surge from happening this year.
Testing
The PCR test output trend over time can be seen in the graph below, represented by the blue line that corresponds with the left y-axis. The red line represents the test positivity rate over time, and corresponds with the right y-axis. The gray dashed line is the goal line for test positivity.
We saw a 17% decrease in PCR testing reported this week. Test positivity continued to decrease and the weekly test positivity rate was 3.1%. The state’s PCR test positivity has been under5% for the past four weeks in a row.
Antigen testing decreased this week, by about 11%, but the positivity rate decreased to 3.7%. Antigen test positivity in Georgia has been below 5% for the past two weeks.
The DPH does not provide data regarding demographic details for cases identified by the antigen test. Keep that in mind as we go through the demographic data in the following sections. You’re only seeing part of the data. Meanwhile, antigen testing identified 28% of the cases this week.
Cases
The number of combined new cases (by date of report) through Sunday is as follows:
- 24 hours: 306 by PCR + 59 by antigen = 365 (+0.03%)
- 7 days: 3155 by PCR + 1223 by antigen = 4378 (+0.4%)
- 4 weeks: 17,929 by PCR + 8,282 by antigen = 26,211 (+2.4%)
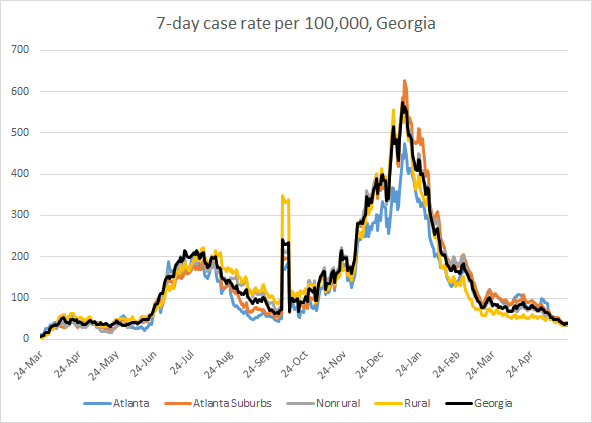
This week cases decreased for all age groups. The 7-day case rate per 100,000 is shown below for the state and for different county types in the state. There is very little variation across county types. Case rate is highest in the Atlanta suburbs, but it’s not that much higher than the state average.
Hospitalizations
The number of new hospital admissions (by date of report) as of Sunday is as follows:
- 24 hours: 18 new COVID-19 admissions, 6 admission to the ICU (weekend reporting is typically light)
- 7 days: 523 new COVID-19 admissions, 122 ICU admissions
- 4 weeks: 2101 new COVID-19 admissions, 430 ICU admissions
As discussed in the combined data section, hospital admissions rose this week. If we look at the demographic data, the admissions rose for nearly every age group.
There is some disagreement between the hospitalization numbers provided by the Department of Public Health and the US Department of Health and Human Services. If we look only at confirmed COVID-19 admissions (this is the same thing DPH tracks) then the HHS age group data look like this for the past week:
There are only two hospital regions in the yellow zone for COVID-19 patient census, regions A and F. Every other hospital region is in the green zone. For ICU bed usage, there are no hospital regions in the red zone.
Deaths
The number of new confirmed deaths (by date of report) is as follows. The percentage in parentheses indicates how the increase compares to Georgia’s cumulative total at the start of each window of time.
- 24 hours: 0 confirmed, 0 probable deaths
- 7 days: 126 (+0.7%), 29 probable deaths
- 4 weeks: 543 (+3.1%), 143 probable deaths
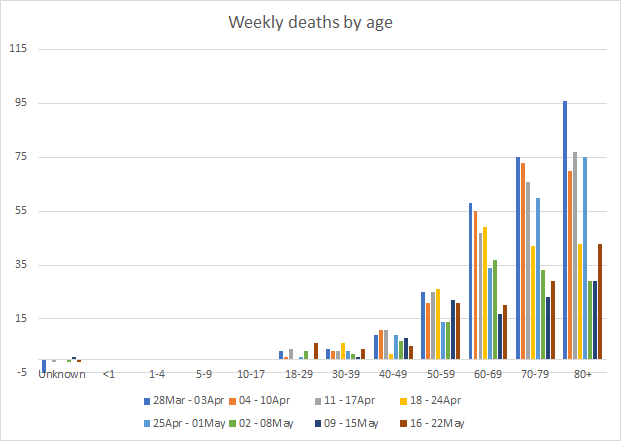
This week, deaths increased for those 18-39, and for all age groups 60+. Remember, these are preventable deaths, especially for the older age groups that were made eligible for vaccination early on. For those who are 18-29, their highest weekly death total has been 8, recorded the week of 07-13February2021. But this week’s total, 6, is tied for the second worst week of deaths. Please don’t confuse youth with protection against the worst that this disease can do. Of the 126 18-29 year olds that have died of COVID-19, only 26% had an underlying medical condition. And we don’t know to what degree those underlying conditions, when they were documented, contributed to their death from COVID-19. Please get vaccinated if you are eligible.
The graph below shows how the different county types in Georgia have been impacted by deaths to date when adjusted for population. Rural counties continue to have the highest death rate and the lowest death rate is observed for the Atlanta counties of Fulton and DeKalb. However, their death rate is similar to the Atlanta suburbs. Nonrural county death rate more or less matches the state average.
Where do we go from here?
I want to apologize for the delay in getting this newsletter out to you. We were able to celebrate my kid’s birthday this weekend with neighbors and family. It was outdoors and all of the adults were vaccinated. Last year we weren’t able to celebrate with family or friends other than via Zoom, so it was important to us to sort of make up for two birthdays in this one. In any case, between that and attending a Kansas City Royals game yesterday (again, outdoors, reduced capacity seating, masks) I was wiped out.
I will say that I’m beginning to feel that the newsletter may need to evolve both for pandemic as well as personal/professional reasons. As for the pandemic, the data are trending downward for Georgia and the nation. If we make it to July without an increase in cases, we might not have a summer surge this year. We are asking the vaccines to do a lot of the heavy lifting these days, even though we have not vaccinated enough people. So while I really hope that we don’t see a summer surge, I can’t exclude that possibility. Professionally, since I plan for both of my kids to resume in-person learning in the fall, I am interviewing for several positions in recent weeks. If I am successful, I may not have as much time to devote to the newsletter.
But the larger truth is that I am really burned out on COVID-19. This doesn’t mean I’m burning my masks or that the pandemic doesn’t matter to me. As I’ve said before, the pandemic won’t feel like it’s over for me until my children are fully vaccinated. Even then, we still need to do the work of ensuring our communities and world are safe too. But I can’t deny that the CDC’s recent change on mask guidance was incredibly demoralizing for me as someone who has been communicating about the pandemic for 15 months. Sort of like, if CDC doesn’t think risk mitigation matters anymore, then why am I still doing this? When the pandemic started, there was a vacuum of good science communication. And a lot of people outside of the agency stepped into that void and began to carry the water for CDC. I don’t mean to presume to be equal to that task, but between myself and the work of dozens if not hundreds of other non-agency public health professionals, I think we communicated the risks and educated the public as best we could - cobbling together a sense of the pandemic from the data sets that were available. But the water has been heavy, and many of us have been carrying the water through minefields of disinformation and politicization. With the change in CDC culture toward the pandemic adding a new challenge, an already difficult (but important) experience has become unsustainable. I need to take some time off and wanted to prepare you guys for that, rather than spring it on you abruptly. My family is going on a multi-state camping adventure starting in mid-June and I may not have reliable access to WiFi during that time anyway. Until that time, I plan to continue at the current tempo. But the newsletter will likely go to weekly distribution during the vacation. Depending on how disease trends are going at that time, I may stick with a weekly COVID-19 distribution.
As part of the generation who grew up playing Oregon Trail, my hope was to get as many people in my wagon (family, friends) and eventually a caravan of my social media following and newsletter mailing list to safety and security as possible. For my family and former students who worked in healthcare, my goal was to keep as many people as possible out of their ERs and ICUs by communicating the risk and how to mitigate it. I couldn’t save someone from COVID-19. I’m not that kind of doctor and don’t have the medical training for that. But I could help to keep them from getting sick in the first place. We still have a lot of work to do to vaccinate as many people as we can. Despite the vaccines being authorized for over 6 months now, we still have significant hurdles when it comes to access. But the need for a Sports Center style commentary on the state of the pandemic may no longer be needed. As a consequence, I am likely going to be shifting content to discussions of current events in public health more broadly. COVID-19 tracking will still be free and accessible to all who wish to read it. But my commentary and analysis of other issues of public health concern, or stories of my experience in the past 15 months will be prioritized for subscribing members. If you wish to be part of that subscriber mailing list, you can become a paying subscriber at the button below. I hope that we can take the lessons learned from this pandemic and grow from them. Among those lessons is a new appreciation for public health and public health data among the general population. If you’ve enjoyed “learning” from me on COVID-19, then let’s continue to stay engaged on science and public health.
References
https://dph.georgia.gov/covid-19-daily-status-report
https://covid-gagio.hub.arcgis.com/
https://beta.healthdata.gov/dataset/COVID-19-Reported-Patient-Impact-and-Hospital-Capa/6xf2-c3ie
Georgia COVID-19 Updates is a free newsletter that depends on reader support. If you wish to subscribe please click the link below. There are free and paid options available.
My Ph.D. is in Medical Microbiology and Immunology. I've worked at places like Creighton University, the Centers for Disease Control & Prevention and Mercer University School of Medicine. All thoughts are my professional opinion and should not be considered medical advice.






Whatever form the newsletter takes in the future, or if it even continues, know that there are many of us out here who are endlessly grateful to the effort you have put in for all of us over the past year. You may not have been on the front line per se, but you’ve done more heavy lifting than most of us in making the data accessible and easy to understand, and that’s no small feat considering the how regularly our understanding of this virus and its impacts have evolved, not to mention the roadblocks to even getting the data (the correct data!) more often than should be necessary. I feel like I could go on and on, but seriously, you’ve more than earned whatever length of break you decide to take. Sincerely, thank you.
I feel demoralized right along with you. I just got home from a trip to Rome and, besides me, saw only two other mask wearers. I hope everyone else was as vaccinated as I was but it's hard to trust.
You are the doctor, one of them, who has gotten me and my family through to this point in the pandemic. We all have pandemic fatigue as well but know that if the virus might not yet be fatigued with us so we continue to mask and take the precautions those of you in public health that did step into the void, taught us to take. I haven't been sick in over a year, nor has anyone in my family-even my internal medicine doc husband who is always sick in the winter.
Some folks are calling all the hand washing and surface cleaning hygiene theater and it may prove unnecessary for the control of Sars-Co-V2, but it was amazingly successful at preventing the spread of influenza this year. I've learned lots of new and valuable life skills!
I hope you and your family have a wonderful trip and I look forward to learning from you in the future in whatever form you chose to share. Safe travels!