Good evening! First, I want to thank those of you who kept your gatherings small, outdoors and socially distant, or who kept things to just their household. I know I had sad moments yesterday when I wished that things were different and we could be with our extended family. So I recognize what an incredible ask it was and an incredible sacrifice. But it’s not a sacrifice without purpose. It is so contrary to human behavior, but it is an act of love to love from afar right now - for our families and for our communities. So thank you, again and again, for sharing that sense of community.
If you did attend a gathering and it was indoors, crowded, masks weren’t really worn, etc, then I am not here to judge you. I understand the deep need for human connection right now. However, I do recommend that you go ahead and make an appointment or plan to seek a COVID-19 test next week. Be sure to communicate your results to the other members of the Thanksgiving gathering, if you are positive.
Second, the Georgia Department of Public Health is still updating their dashboards, which means there is probably a number of folks who did not have yesterday off from work. Neither did some of the laboratorians, since our testing numbers are pretty robust today. And, of course, the doctors, nurses, respiratory therapists, pharmacists and others who care for the ill in our hospitals didn’t take the day off either. So, again, thank you to all who are sacrificing for their communities this week.
Testing
Today there were 31,722 new PCR test results reported, a mid-range day for us. That’s unexpected, given that yesterday was a holiday, many laboratories were closed, specimen collection centers were closed, etc. I think many of us were expecting weekend effect and we do see that for hospital admissions, but not for any of the other metrics. Of today’s new tests, 8.3% were positive. That’s above the goal of 5% but if you look at the graph below that shows the Georgia percent positive rate each day over time, we really aren’t that far away from the 5% goal. Of course, with antigen tests making up a substantial portion of each day’s cases, the percent positive rate for PCR is diminishing in value as a metric for assessing how Georgia is doing in the pandemic.
Cases
There was a net increase of 2394 newly reported PCR cases and 615 newly reported antigen cases to result in a combined increase of 3009 for the day. Again, it’s a bit strange to see the numbers this high, given the holiday. In any case, the new total number of cases is 464,526 (416,303 by PCR, 48,223 by antigen test). Of today’s newly reported cases, 32% came from the nonrural counties outside of the Atlanta metro, 27% came from the Atlanta suburbs, 16% came from rural counties and 15% came from the Atlanta counties of Fulton and DeKalb.
The school-aged data surveillance report has not been released yet by DPH and it might be delayed or skipped entirely due to the holiday. In the meantime, I’d like to discuss an open records request that I recently got back from the Department of Public Health regarding disease clusters. In total, there have been 3265 total clusters identified to date, associated with 29,179 cases, 2165 hospitalizations and 1652 deaths as of 23Nov. In other words, that’s 6.4% of the cases, 6.4% of the hospitalizations and 19.1% of the deaths reported for the state of Georgia as of 23Nov. This indicates that contact tracing efforts have not been sufficient to identify links to other cases (probably due to a shortage of workers), but another contributor is just widespread disease that is unchecked in our communities.
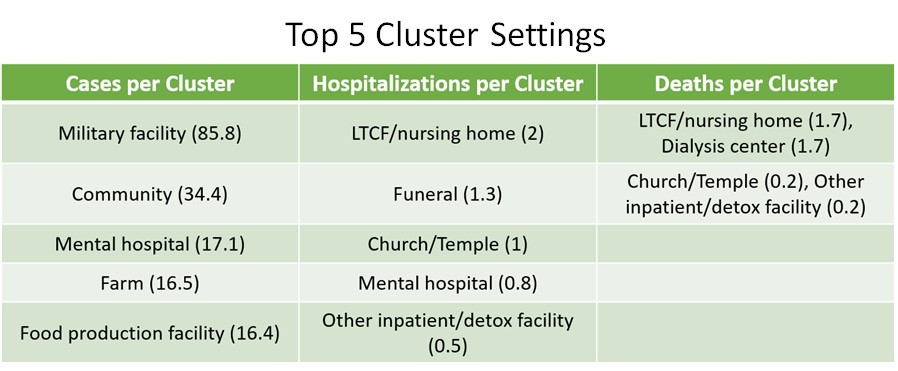
First, here is a table that shows the top five cluster settings in terms of number of clusters, number of cases, number of hospitalizations and number of deaths. The number in the parentheses tells you the number identified.
You’ll probably notice right away that Long Term Care Facilities (LTCFs) dominate every category. But it may surprise you to know that schools are the number two setting for number of clusters and number of cases, especially considering they’ve only been meeting in person (and only for some of the school districts) since August. It may also surprise you that church/temple is the number two cluster associated with hospitalizations and deaths. This next table takes these numbers from raw counts to the average number of cases, hospitalizations and deaths per cluster for a given setting. The top five are presented below. I should note that the data given to me in the open records request was heavily redacted so it wasn’t possible to calculate the ratio for every setting. It’s policy to redact anything with a count equal to or less than 5 to avoid identifying a particular business, school, or other setting.
It was really astonishing to see that although LTCFs are associated with a high cluster county and a high case count, on average, they only result in 15.3 cases per cluster and don’t even make the top 5. Military facilities top the list, so although they have relatively few outbreak clusters (n = 8), the disease spreads like wildfire through that setting. LTCFs take the lead for average hospitalizations per cluster as well as deaths per cluster (equal to dialysis centers). This probably has to do with the advanced age and possibly poor health status of their residents, at least, more so than in the general population.
Hospitalizations
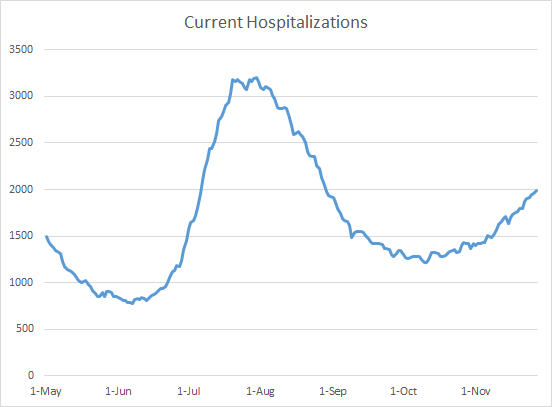
As I mentioned in the testing section, the only place where we are seeing something that looks like holiday effect is in the hospitalizations reported today. There were only 18 new hospital admissions reported today and 1 admission to the ICU. Those are numbers more reminiscent of our weekend numbers.
However, the number of patients currently hospitalized for COVID-19 jumped to 1985, 28 more than yesterday.
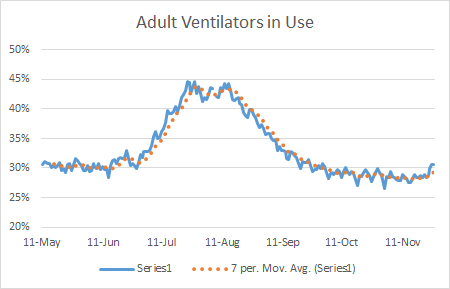
Another thing that’s interesting is that the percentage of ventilators that are in use has increased to 31%. However, I think this is a combination of factors. The number of total ventilators in use has increased over the past two weeks and especially in the past three days. But the number of available ventilators has decreased in the past four days too, possibly because the staff that support those beds are taking a well-deserved break for Thanksgiving. We aren’t in a danger zone or anything here, I just wanted to discuss this in more depth in case anyone was seeing that percentage rise and beginning to get concerned. I wouldn’t be surprised if that number goes back down on Monday, but we’ll have to wait and see.
Deaths
It was a medium-low kind of day for deaths with a net increase of 30 deaths today compared to yesterday’s total. Of those deaths, 12 came from nonrural counties outside of the Atlanta metro, 9 came from the Atlanta suburbs, 7 came from rural counties and 1 came from DeKalb county (Atlanta).
The graph below shows the relationship between cases and case fatality rate. The cumulative number of cases is presented by the gray line, corresponding to the left y-axis. The noise in the line is due to the inclusion of antigen cases that were reported weekly for a time. The case fatality rate, or how many deaths there are per cases is represented by the blue line and corresponds to the right y-axis.
When the summer surge happened (see around 11Jul), cases increased at a faster rate than before and the case fatality rate (CFR) dropped like a stone as a result as deaths were diluted by the influx of cases. However, deaths began to rise about three weeks after the case surge began (data not shown) and that halted the drop in the CFR. It increased slightly, but has held steady for the past three months. Lately, though, it’s started to decrease again as our cases have grown at a faster rate again, both due to the inclusion of antigen cases and because disease transmission has grown in general. So we’ll have to see how far the CFR drops this time and whether the pattern repeats.
That’s it for today. Have a great weekend and I’ll be back on Sunday!
References
https://dph.georgia.gov/covid-19-daily-status-report
https://covid-gagio.hub.arcgis.com/
Georgia COVID-19 Updates is a free newsletter that depends on reader support. If you wish to subscribe please click the link below. There are free and paid options available.
My Ph.D. is in Medical Microbiology and Immunology. I've worked at places like Creighton University, the Centers for Disease Control & Prevention and Mercer University School of Medicine. All thoughts are my professional opinion and should not be considered medical advice.