Vaccine Update
Here's a link for healthcare workers to register for an appointment to get their vaccine if they are not part of a larger hospital system that is providing them (https://dph.georgia.gov/provider-vaccine-registration-ph-district-list).
This week, vaccination eligibility has expanded to first responders and people >65 years of age although the rollout is not without problems. DPH has provided this vaccine locator so that you can find the enrolled vaccine providers in your area and make appointments, if vaccine is available.
We can see how the US (and Georgia) is doing with respect to the vaccine administration effort using the CDC’s COVID-19 Data Tracker. Nationally, 34% of the available doses have been used to initiate a person’s 2-dose vaccine series. Of those who have started the vaccine series, 15.2% have had their second dose.
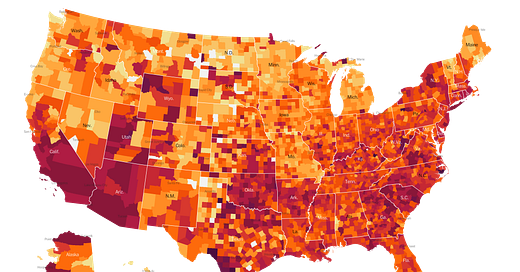
The CDC Tracker provides a map of the US for how many people have received at least one dose of the vaccine, adjusted for population. Using this method of looking at vaccine data, Georgia’s vaccination rate has increased 71% in the past week. For the state, 204,301 people have initiated the two-dose series. 22,324 people have completed the 2-dose series in Georgia. It is great to see that upward momentum. However, Georgia is still ranked last among the 50 states, with a vaccination rate that is 1,924 per 100,000 residents. To be fair, someone has to be last. That’s how numbers work. But it’s a shame to see that the states with the poorest vaccination rates are all in the South. States with more rural populations than ours have been able to vaccinate more of their population. In fact, the top three states for doses administered per 100,000 residents are West Virginia (6307), Alaska (5406), and South Dakota (5307). The bottom three states are Alabama, Georgia, South Carolina, Idaho and California. In other words, West Virginia has vaccinated more than twice as much of their population as Georgia has, but last week it was 3x higher. So Georgia is narrowing the gap, despite being ranked the 49th state in the nation.
I know there are legitimate concerns about safety with the new COVID-19 vaccines. If you have questions about how the vaccines work or vaccine efficacy, please check out this newsletter I wrote. The clinical studies showed that the most common side effects were similar to what you see with the flu vaccine, things like pain at the injection site, fever, fatigue, headache, etc. Many of these things are signs of inflammation - your immune system is responding to something new - exactly what we want your immune system to do with a vaccine. As the vaccine is used more widely in the population, any adverse events are reported through the Vaccine Adverse Event Reporting System. The data are available to the public and updated on Fridays. A couple reminders, these events are reported and pending investigation to determine whether the adverse event was due to the vaccine or an unrelated cause.
I sorted the search criteria to limit it to events considered serious and associated with an emergency room visit. So far there have been 165 people that fit these criteria and the top symptoms experienced are listed below. There are 1453 symptoms listed. Just keep in mind that people can experience more than one symptom at once. Some of the “symptoms” are laboratory results, including normal findings. Also, some of the symptoms are redundant depending on how the report was submitted. For example, tachycardia means elevated heart rate. But if the person submitting the report said “heart rate increased,” then that’s a separate symptom listed even though they’re the same thing. So these things explain why there’s a disagreement between 165 and 1453. Two of these medical terms will be unfamiliar. Dyspnoea = shortness of breath, pyrexia = fever.
As of Friday, there have been 165 people with serious events associated with an ER visit out of 12.2+ million people who have started the vaccine series (or 0.0013%). And not all of those will ultimately be determined to be associated with the vaccine. But even if this is the worst case scenario and all of these were definitively linked to the vaccine, the vaccine continues to be very, very safe for the larger population so far. That’s reassuring news, and I’ll be sure to keep an eye on this to let you know if there are big deviations. Important caveat: both data collection streams might be susceptible to delayed reporting.
The World
According to the New York Times Coronavirus Tracker, the SARS-CoV-2 virus that causes COVID-19 disease has sickened >95.1 million people (+4.8 million since last week) and killed at least 2,031,700 (+96,000 in the past week) worldwide as of this morning.
The US is ranked in the second highest color category for hot spots. We are ranked #11 in the world for average daily case rate per 100,000 people over the past 7 days (last week, #10) with a rate of 66 compared to 77 last week. So our case rate has improved. The top five countries for average daily case rate per 100,000 in the past week are Gibraltar, Andorra, Portugal, Israel and Czech Republic.
For deaths, the US average daily death rate per 100,000 over the past week is 1.0 (previous week was 0.98), and we are ranked #15 in the world for this (last week we were ranked #16). The top five countries for average daily death rate per 100,000 in the most recent week are Gibraltar, United Kingdom, Czech Republic, Portugal and Slovakia.
The United States
The map above comes from the New York Times Coronavirus Tracker. As of this morning, there have been over 23.9 million cases (+1.5 million in the past week) and 397,612 deaths in the US (+23,184 in past week). Keep in mind that both of these numbers are probably an under-count of the situation in our country.
This week we see less intensity throughout the map than the previous week. According to data from the 17Jan21 HHS Community Profile Report (the source document for the White House Coronavirus Task Force reports), the top five states in the nation for new case rate per 100,000 residents are Arizona, California, Rhode Island, South Carolina, and Arkansas. In addition to South Carolina in the top 10 - in Georgia is ranked #8. The top five states in the nation for average daily death rate in the past 7 days are Arizona, Alabama, Kansas, Mississippi, and Pennsylvania. Tennessee is ranked #8 and Georgia is ranked #13 (last week #37) for 7-day death rate per 100,000.
The table below tells you where we are this week and how that compares to the previous week (in parentheses). The data for everything comes from the HHS Community Profile Report from 17Jan2021. Keep in mind that some states did a lot of catching up with delayed reporting due to the holidays last week, so the rankings might not be accurate assessments of how states compare this week.
Georgia has seen a dramatic increase in its ranking for death rate per 100,000. Georgia currently does not have any counties in the list of the top 20 counties for disease rate in the nation.
Influenza-like illness in the US remains very low, but this week we are seeing higher level of minimal activity in the same areas of the country that are surging with COVID-19. You can consult FluView any time you’d like to see this map and other data visualizations. You can read the weekly report from Georgia Department of Public Health here.
Georgia
Normally, in this part of the newsletter I would give you an updated risk map for Georgia, calculated and formatted in the same way as the Brown University School of Public Health but including Georgia’s antigen cases (which DPH does not for any of their graphs or maps). Evidently the person responsible for this tool moved from Harvard to Brown. However, the map isn’t particularly interesting this week since the entire state is in the red category, all 159 counties.
Let’s discuss today’s numbers for Georgia.
Testing: a robust day for PCR testing, especially considering it is a Monday. There were 31,865 new PCR results reported, 16% of which were positive. Antigen testing identified 12% of today’s cases.
Cases: cases are often lower on Mondays due to weekend effect. Today there was a net increase of 4957 newly reported cases (4385 by PCR, 572 by antigen test). Of today’s newly reported cases, 34% came from nonrural counties outside of the Atlanta metro followed by 31% coming from Atlanta suburbs. For the first time in a while, there were more cases reported today from Atlanta (19% of cases) than from rural counties (15% of cases). The top five counties for 14 day case rate are Madison (3519), Taliaferro (2342), Warren (2208), Treutlen (2087) and Jackson (1871). Other than Jackson county (nonrural), these are all rural counties.
Hospitalizations: there are 5,552 patients currently hospitalized for COVID-19. This is a small increase compared to yesterday, but 63 fewer patients than a week ago.
COVID-19 patients represent 33.3% of all patients currently hospitalized in Georgia and this varies by hospital region. In 6 of the 14 hospital regions in Georgia, COVID-19 patients represent >40% of all patients currently hospitalized. Georgia is #3 in the nation for this metric behind California and Arizona.
More than 91% of the ICU beds in the state are full. According to HHS, 49% of Georgia’s ICU beds are occupied by COVID-19 patients. The demand this disease is placing on our healthcare system is intense. Four regions are coping with an overage, regions A, E, G and M. Twelve regions (of 14) are using >90% of their ICU beds.
There were 122 new hospital admissions for COVID-19 today and 7 admissions to the ICU. We typically see lower numbers on Mondays.
Deaths: there were 63 newly reported confirmed deaths compared to yesterday’s total. Death reporting on Mondays is typically low due to weekend effect. So seeing a number like 63 on a Monday is a lot. For today’s deaths, nonrural and rural counties outside of the Atlanta metro each contributed 33% of them. Nineteen percent of today’s deaths came from the Atlanta suburbs and 10% came from the Atlanta counties of Fulton and DeKalb. The state 7-day death rate per 100,000 residents is 38% higher than the summer peak.
References
https://covid.cdc.gov/covid-data-tracker/#vaccinations
https://beta.healthdata.gov/download/gqxm-d9w9/application%2Fpdf
https://dph.georgia.gov/covid-19-daily-status-report
https://covid-gagio.hub.arcgis.com/
Georgia COVID-19 Updates is a free newsletter that depends on reader support. If you wish to subscribe please click the link below. There are free and paid options available.
My Ph.D. is in Medical Microbiology and Immunology. I've worked at places like Creighton University, the Centers for Disease Control & Prevention and Mercer University School of Medicine. All thoughts are my professional opinion and should not be considered medical advice.