This week we are seeing exponential growth of cases and some regions are seeing exponential growth in COVID-19 patient census in the hospital. Let’s dig in. First, here’s how the four big metrics are trending, week by week.
This week, cases rose 85% compared to the previous week. Hospital admissions for COVID-19 rose 66%. ICU admissions rose 8% and deaths are nearly the same, rising 4% compared to the previous week.
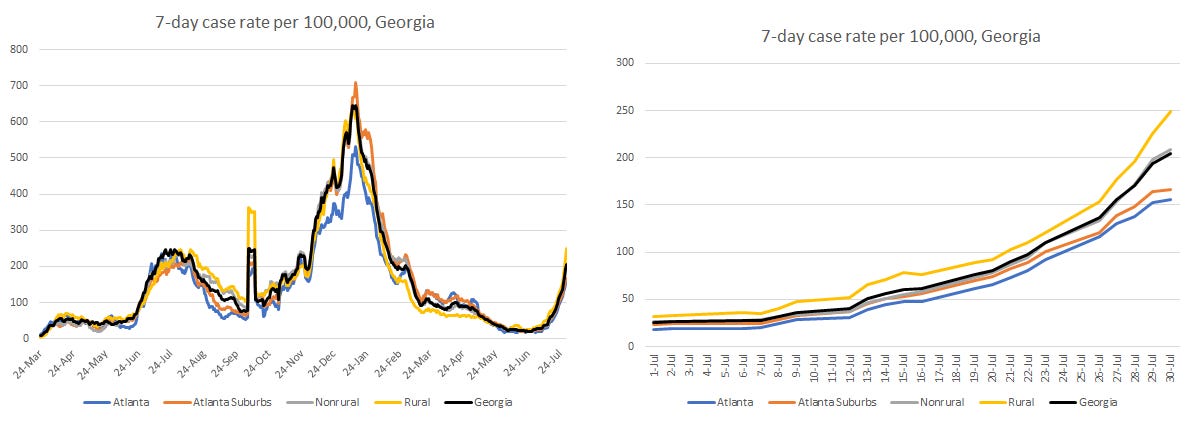
Case rate per 100,000 nearly doubled in the past week for rural and nonrural counties outside of the Atlanta metro. That doesn’t mean that Atlanta and its suburbs aren’t rising, just not as fast. The 7-day case rate per 100,000 is approaching our peak during the summer surge of 2020.
We can also see this dramatic rise when we look at how cases from the week compare across age groups (PCR-identified cases only). Cases rose for all age groups and the ‘unknown’ category also rose, indicating that contact tracers are now starting to be overwhelmed.
Not only are cases and case rates growing more intense, but because test positivity is above 5% for both PCR and antigen testing it means that the state is no longer able to see how big the problem is. This week testing rose for both PCR and antigen testing (blue lines for each graph below. But the test positivity for both rose even more. Of the tests performed this week, 11.9% of PCR tests were positive and 12.9% of antigen tests were positive.
We can also see how PCR test positivity varies across age groups in the state. For any age group with a bar over 5%, we are missing cases. We are likely missing a lot of cases among children aged 5-17, or K-12 aged children. With children of this age group about to start school next week, and some districts not requiring masks at all and some saying no one is quarantining this year even if positive, we should expect both cases and test positivity among kids to surge even higher.
Meanwhile, childrens hospitals in Kansas City (where I live), Baton Rouge, New Orleans are surging with children needing hospitalization and intensive care for COVID-19. In Oklahoma, there are no pediatric hospital beds available in the state. Next door in Arkansas, childrens hospitals are also feeling the strain with kids in the ICU for COVID-19. From next door in Alabama:
“I’m scared,” said Dr. David Kimblerin, co-director of the division of pediatric infectious diseases at UAB and Children’s of Alabama, during a Facebook Live hosted by the Medical Association of Alabama. “I was uncomfortable last year but I am scared right now for what lies in front of us with respect to our children.”
“This delta strain is different and it is bad,” he said of the COVID-19 variant’s high transmission rates, which make it more likely for both vaccinated and unvaccinated people to get ill and pass the virus on to others. “We are standing in a tunnel right now and the train is accelerating at us as we speak.”
And we can see that this situation is starting to appear in Georgia too. The graph below comes from the Georgia DPH School Aged Surveillance Report. It shows that ER visits for COVID-19 are skyrocketing among kids of all ages.
So when this starts to happen in a bigger way in Georgia and kids who were previously healthy are on ventilators, I don’t want school superintendents to claim that there was no way this could have been predicted. We have plenty of warning that the situation in 2021 is more dangerous than a year ago for children. Willingly choosing to endanger children by not doing the bare minimum of disease control and prevention should be treated the same way as knowingly allowing someone drunk to drive a school bus and organizations that do so should be held to account. They don’t get to push the blame to someone else after they dismiss CDC guidance. Georgia children are going to end up in the hospital or worse. In addition, they will go home to families where they spread the disease to others, some of whom may be immunocompromised (think pregnant moms - it’s more common than you think), older grandparents, and others with underlying medical conditions. The liability alone would scare me enough as a superintendent to enact a mask mandate at the elementary level at the very minimum where none of the kids are eligible for a vaccine. Georgia is special for many good reasons, but the state doesn’t have special protection against the things happening to kids in other states happening to Georgia kids too.
I’m fielding questions to the effect of “how bad do we expect this to get?” Some have a mistaken impression that this will be a quick burst of disease that dissipates in time for the college football season (I wish). Start by looking at Missouri, where delta first took hold (lower left). Their hospitalizations have been climbing since early June and are still climbing with no real sign of leveling off. That’s two months of sustained growth. Alabama, Georgia and Florida are only a month into their surge.
We can maybe make predictions based on what happens in Missouri. For example, if they reach a peak soon we could estimate a 2-2.5 month climb in other states. But Missouri’s vaccination rate is higher than many of the southern states (exceptions being Florida). So what happens in Missouri might not predict what happens in the South. Florida’s hospitalizations are nearly at the same level as the winter surge peak, and continuing to climb. What many of these states have in common is that they’re not really doing anything to halt the spread of disease - letting the disease burn through their communities. They’re also not doing much to augment their healthcare infrastructure. So they’re not preventing illness and not helping hospitals to cope with the disease burden. Citizens are literally on their own against an invisible threat.
The map on the right shows the percent of the population that is fully vaccinated by county, using data from today from Georgia Department of Public Health. The top county in the state is still Oconee (51.1%), but Oconee hasn’t really added much since the last time I graphed this in early July. We have seen improvement in the southeast corner of the state, which was previously all the white color. Mind you, at 51.1%, even the highest performing county is well below where we need it to be.
But that cluster of most vulnerable counties in the southeast corner of the state is showing us the danger of a low vaccination rate meeting the delta variant. Hospital region J (Savannah and the Georgia coastal area) has been seeing exponential growth in patient census, and the same is observed for region M (Waycross and surrounding counties). Region J is not far from the maximum experienced in the summer 2020 and winter 2020-2021 surges. And this is before schools and colleges reopen for the fall semester. For region M, they’re about halfway to the maximum experienced in winter of 2020-2021. How soon before these hospital systems are so overwhelmed that there is no bed for a heart attack, car accident, or other problems?
There’s a lot to talk about when it comes to the CDC’s sudden about face on mask guidance, breakthrough infections and the data that supported that decision related to the increased transmissibility of the delta variant. But this newsletter is getting a bit long at this point. I plan to write about the CDC guidance and data tomorrow.
The COVID Digest is a free newsletter that depends on reader support. If you wish to subscribe please click the link below. There are free and paid options available.
My Ph.D. is in Medical Microbiology and Immunology and I am Chair of the Division of Natural Sciences and Mathematics at the University of Saint Mary. I've worked at places like Creighton University, the Centers for Disease Control & Prevention and Mercer University School of Medicine. All thoughts are my professional opinion, do not represent the views or opinions of my employer and should not be considered medical advice.











Is there any data if the teenagers (12yo+) that are being admitted are vaccinated or unvaccinated?